We want to ensure that you receive the highest level of healthcare. This means keeping you educated and informed about what is involved in the different stages of a Endoscopy procedure. If you have any questions or concerns, please speak with your doctor or medical technician.
Understanding Endoscopies
An Endoscopy is a day care procedure (you return home on the day of the procedure) which is done by introducing a thin, flexible tube with a camera and light source (endoscope), to visually inspect the body’s interior. It enables medical professionals to examine and evaluate inside organs, tissues, and structures without invasive surgery. An Endoscopy gives real-time visualisation during medical procedures.
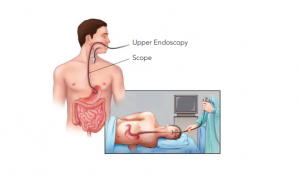
Why is an Endoscopy Done?
An Endoscopy may be done to:
Investigate symptoms
An endoscopy can help determine what’s causing digestive issues such as heartburn, nausea, vomiting, abdominal pain, difficulty swallowing, and gastrointestinal bleeding.
Diagnose conditions
An Endoscopy allows the collection of tissue samples (biopsy) to test for diseases and conditions that may be causing anaemia, bleeding, inflammation or diarrhoea. It can also detect some cancers of the upper digestive system. An Endoscopy is sometimes combined with other procedures, such as an ultrasound. An ultrasound probe may be attached to the endoscope to create images of the wall of your oesophagus or stomach. An endoscopic ultrasound may also help create images of hard-to-reach organs, such as your pancreas. Newer endoscopes use high-definition video to provide clearer images.
Treat digestive issues
Special tools can be passed through the endoscope to treat problems in your digestive system. For example, an Endoscopy can be used to burn a bleeding vessel to stop bleeding, widen a narrow oesophagus, clip off a polyp or remove a foreign object.
How to Prepare for Your Endoscopy
Your provider will give you specific instructions to prepare for your Endoscopy. Fast before the Endoscopy You’ll typically need to stop eating solid food for eight hours and stop drinking liquids for four hours before your Endoscopy to ensure your stomach is empty for the procedure. On the day of the procedure, make sure that you do not eat anything and follow the instructions given by the anaesthetist regarding your routine medications.
Special Instructions
Kindly inform us if you are allergic to any medications or substances. It is important that we are aware of any history of abdominal surgeries, bleeding disorders, intake of antiplatelets (aspirin, clopidogrel etc.), anticoagulants (warfarin, acitrom, apixaban, dabigatran etc.), blood thinners or long-term anti-inflammatory medications. Arrange for someone to pick you up from the hospital. Don’t drive, make important decisions or go back to work for the rest of the day. You may be advised to avoid driving for 24 hours following the procedure.
During the Endoscopy
-
You will be admitted 45- 60 minutes before your procedure, unless otherwise advised by the patient care coordinator. After check-in, a Health City team member will lead you to a room where you can change into a hospital gown. A nurse will check your vitals such as blood pressure, pulse, and oxygen levels, and place an IV line into your arm to begin delivering sedatives and pain medication to your bloodstream. From there, you will be taken inside the scopy room for your procedure.
Step 1
-
You’ll begin the exam lying on your back or on your side. As the procedure gets underway:
-
Monitors are often attached to your body.
-
This allows our healthcare team to monitor your breathing, blood pressure, and heart rate.
-
You may receive sedative medication.
-
This medication, given through a vein in your forearm, helps you relax during the Endoscopy. Most people undergoing an upper Endoscopy will receive a sedative to relax them and make them more comfortable during the procedure.
-
An anaesthetic may be used in your mouth.
-
An anaesthetic spray numbs your throat in preparation for insertion of the endoscope. You may be asked to wear a plastic mouth guard to hold your mouth open.
-
The endoscope is inserted in your mouth.
-
It will travel down your oesophagus but won’t interfere with your breathing.
-
A tiny camera at the tip transmits images to a video monitor in the exam room.
-
Your provider watches this monitor to look for anything out of the ordinary in your upper digestive tract. If something unusual is found, images can be taken for later examination.
-
Gentle air pressure may be fed into your esophagus to inflate your digestive tract.
-
This allows the endoscope to move freely, and it allows the folds of your digestive tract to be examined more easily. You may feel pressure or fullness from the added air.
-
Your provider will pass special surgical tools through the endoscope to collect a tissue sample or remove a polyp.
-
This is done with help from a video monitor to guide the tools. When the exam is finished, the endoscope is slowly retracted through your mouth. An Endoscopy typically takes 15 to 30 minutes.
Step 2
-
After the Endoscopy, you’ll be taken to a recovery area to sit or lie quietly. Our healthcare team will monitor you as the sedative begins to wear off.
Step 3
Frequently Asked Questions
During your Pre-Anaesthesia Clinic appointment, discuss with your anaesthetist if general anaesthesia (a controlled loss of consciousness, like sleeping) or conscious sedation (a depression of awareness where you might fall asleep or stay awake) is more suited for you.
During the procedure, you might feel uncomfortable but it shouldn’t hurt. A general anaesthetic or sedative will make you relaxed and an anaesthetic spray will numb your throat. The doctor may use a plastic guard to keep your mouth open and ask you to swallow while the scope is placed in your throat. It might feel like pressure, but not pain. Afterward, you might feel a bit bloated, gassy, or have some stomach cramps.
An Endoscopy is a very safe procedure. Rare complications include: Bleeding: Biopsies or treatments for stomach disorders during an Endoscopy increase bleeding risk. Rarely, bleeding may be severe, requiring a blood transfusion. Infection: Endoscopies typically involve examinations and biopsies, posing a low risk of infection. However, the risk increases with additional procedures, though most infections are minor and can be managed with antibiotics. Tearing of the gastrointestinal tract: Oesophageal or upper digestive tract tears are rare but may require hospitalisation or surgery. They occur in approximately 1 out of 2,500 to 11,000 diagnostic upper endoscopies. A reaction to sedation or anaesthesia: This is low-risk. Call your healthcare provider immediately or go to an emergency room if you experience any of the symptoms below: • Fever • Chest pain • Shortness of breath • Bloody, black or very dark colored stool • Difficulty swallowing • Severe or persistent abdominal pain • Vomiting, especially if your vomit is bloody or looks like coffee grounds






